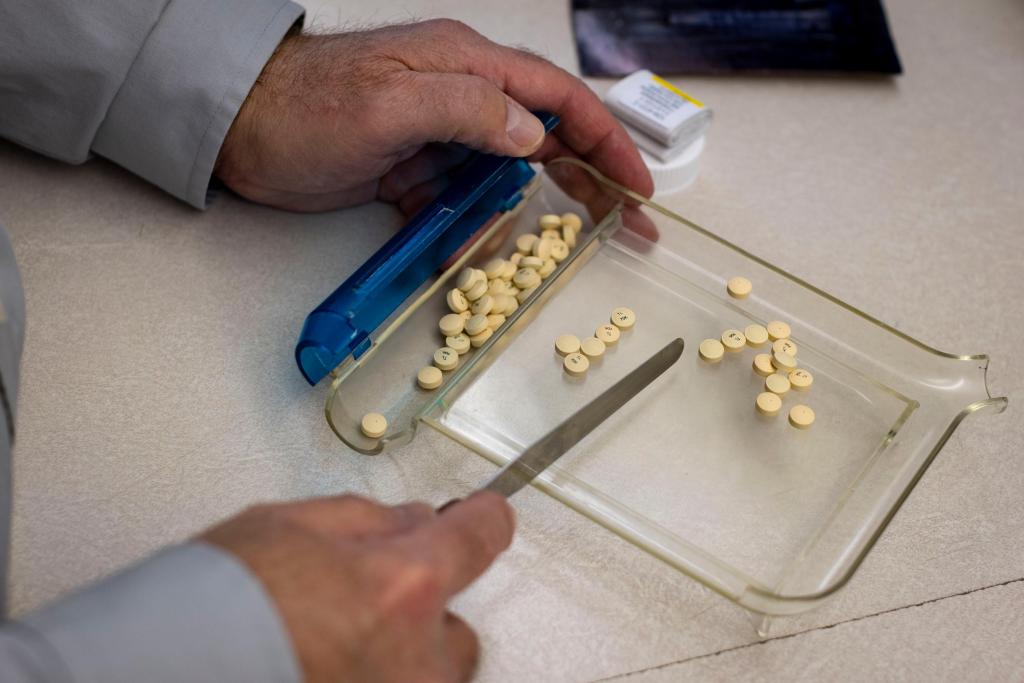
Colorado grew to become the primary state within the nation Friday to set a most value that insurers and sufferers will pay for a prescription treatment — a transfer that’s more likely to face lawsuits.
The state’s Prescription Drug Affordability Board voted to set a most value of $600 for 50 milligrams of the arthritis drug Enbrel. Adults sometimes take that dose weekly, for an annual most value of about $31,200. Youngsters with juvenile arthritis take about half that quantity, placing their most at roughly $15,600.
As of 2023, insurance coverage firms in Colorado paid a median of about $53,000 a 12 months for every buyer utilizing Enbrel. Sufferers paid about $4,600 yearly out of pocket, on common, for the treatment.
The drug treats six autoimmune situations, which contain the immune system attacking joints, pores and skin and different tissues.
The board set its value primarily based on Medicare’s “most truthful value” of about $584, which is the value the federal Facilities for Medicare and Medicaid Providers provided as a part of value negotiations. By regulation, CMS has to think about the price of producing the drug, whether or not the producer has recouped its funding to develop the treatment, how a lot federal assist it acquired for growth and gross sales information, amongst different components.
Final 12 months, the board voted to deem Enbrel “unaffordable,” establishing a months-long means of figuring out whether or not it ought to set a value ceiling, and, in that case, how low it needs to be. The board discovered the drug’s wholesale value had elevated greater than 1,500% because it debuted in 1998 and about 40% over the earlier 5 years.
Amgen, which makes Enbrel, sued the state following the board’s determination final 12 months. A federal decide threw out the lawsuit in March, discovering the corporate hadn’t confirmed it could endure any hurt. Amgen must present that the utmost the state will permit insurers to pay is low sufficient that the wholesalers the drugmaker sells to would want to pay much less, Choose Nina Wang dominated.
Now that the state has set a value, Amgen might sue once more and argue that the value is just too low.
Rae Wall, of Denver, informed the board Friday {that a} value ceiling would ease stress on her household and others with persistent diseases.
“I’m all too conversant in what it’s wish to battle to afford lifesaving medication, having to determine whether or not or not I spend my grocery funds for the complete month on a refill,” she mentioned.
The Pharmaceutical Analysis and Producers of America known as the higher cost restrict a “reckless experiment” that wouldn’t handle the drivers of excessive prices for sufferers.
“Colorado is risking affected person entry and jeopardizing the event of recent medicines — just like how Medicare beneficiaries are going through fewer choices, extra remedy denials and better prices underneath the Inflation Discount Act,” spokesman Reid Porter mentioned. “Mimicking this flawed mannequin won’t safeguard affected person entry and affordability from these abusive practices by middlemen.”
Whereas drug firms have raised considerations about entry, nobody is aware of if they’d really minimize off gross sales to at least one state, significantly if the utmost value remains to be greater than the fee to provide the treatment. That value data is proprietary, so the general public can’t examine it to the higher cost restrict.
What a person pays for drugs is dependent upon their insurance coverage plan. Some plans require a flat copay, and folks with that sort of protection doubtless gained’t see any change of their out-of-pocket prices. Others require their clients to pay a proportion of the price of their treatment. In these instances, sufferers might see their prices go down.
Join our weekly publication to get well being information despatched straight to your inbox.
Initially Printed: